Accountant-Turned-Critical Care Nurse is on the Front Lines
Touro Alum Benjamin Korman Discusses His Nursing Career and Life in the ICU During Pandemic
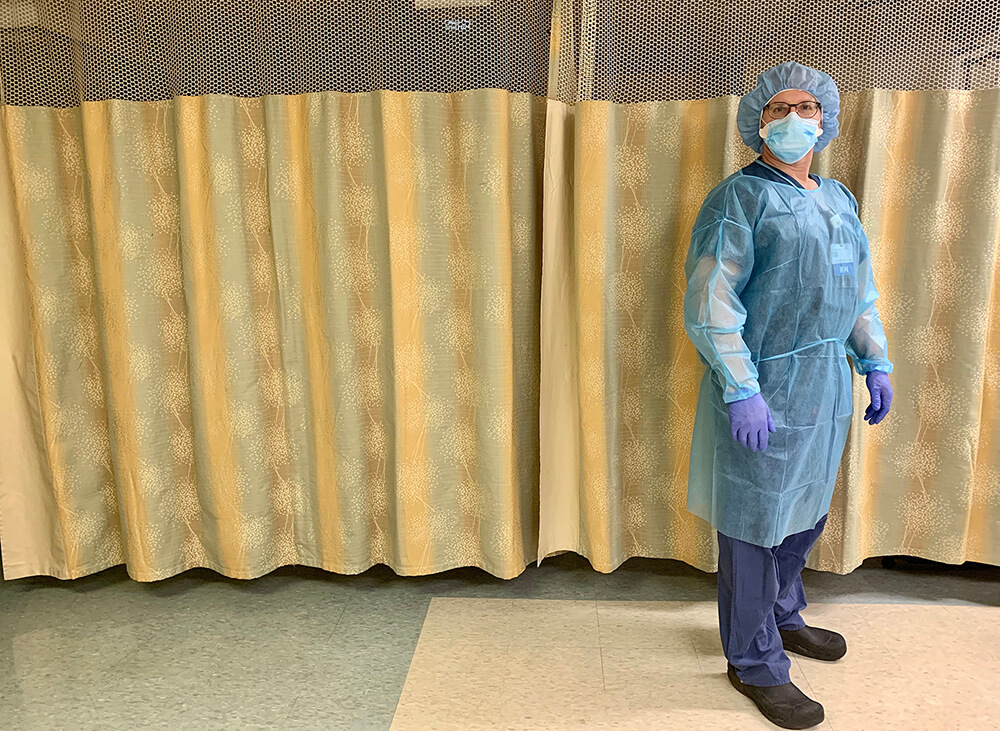
You switched careers from Accounting to Nursing – what prompted the career change?
I was working as an accountant and not finding great fulfillment in that role when I got into a motorcycle accident that changed my life. I went from managing my workload in an office to being completely dependent on nurses. I was in very bad shape and experienced a lot of pain as a result of “road-rash” and fractures. The nurses were so kind and caring and they literally saved me. I had a lot of time to think about life at that point and all I could think was, “Wow, what an incredible job they have. I want to do that as well. Why shouldn’t I have a job that’s so rewarding?”
It wasn’t easy because I was married with two kids at the time; however, my wife was very supportive. As soon as I recovered, I enrolled in Touro again, this time for a bachelor’s in biology before heading to nursing school. Today, I can honestly say that every day is a beautiful day. Although the work is often challenging and extremely stressful, I truly love every minute. I feel so gratified that I can spend my days having a tremendous impact on the lives of patients and families. My goal every day is to try to go beyond what’s expected, for all my patients – comforting a child with epileptic seizures, encouraging and educating families of stroke or cardiac arrest patients and the list goes on. The rewards are truly priceless. Driving to the hospital; I pray that I will be able to do the best I can for each and every patient.
Can you describe a day in the life of an ICU nurse during the COVID-19 pandemic?
In two words, I would say it’s “controlled chaos.” Our administrators at Northwell Health Forest Hills Hospital are excellent and have created team structures and procedures. The number of patients varied from day to day, and they’ve now converted multiple other units into ICUs. There is so much to monitor and it’s all critically important – sedation, blood glucose levels, blood pressure, antibiotics, hydration and nutrition. The number of medications and drips per patients vary and is part of a complex package compiled specifically for each patient at a given time, yet things can and do change in a New York minute. The patients’ survival depend on so many factors, with the entire health care team working cohesively on a constant basis. Many COVID patients suffered from hypotension, or low blood pressure, and kidney failure. It’s a delicate balance we have to strike, since a somewhat stable blood pressure is required in order to start dialysis which treats the kidney failure. In other words, when a patient’s blood pressure is too low, dialysis is generally not an option until the issue is corrected.
What do you find most challenging?
Going to work knowing we are risking our lives for others is quite a challenge, and seeing people in their 30s and 40s coming in with COVID and even passing away. I can’t deny it – these are frightening times. Keeping it together, both mind and body, during this pandemic, is a challenge for health care professionals. We see so much pain and suffering but we can’t let it break our spirits. I have been attempting a strategy used by a senior trauma nurse to keep my mental health intact. When something goes on at work, I place it in a bag in my brain. Before I go into my house after my 12- or 16-hour shift, I hang the bag up on a hook outside my home. I do everything in my power NOT to take any pain into my home.
What is most rewarding?
Seeing patients improve and actually go home. While the day-to-day reality of caring for sick people is rewarding as well, seeing the results of our efforts when they actually recover is immensely rewarding. Being part of the front-line team is amazing. Every single employee at the hospital is part of the front-line team. We are all putting ourselves at risk to keep taking care of patients and keep the hospital employees and visitors safe. In the ICU, we monitor patients constantly and can never let our guards down for even one minute. The only way to achieve this goal successfully is to work as a cohesive team. Nurses, doctors, respiratory therapists, dietary, radiology, pastoral, social workers transport, security, pharmacy, laboratory, materials, management/administration, just to name a few – we all collaborate to create a plan and do the best for our patients and staff.
How did Touro help with your career?
My B.S. in Biology gave me a very strong science background, which of course helped me become a better nurse and enabled me to understand the anatomy and physiology, chemistry, pharmacology and disease process.
Beyond that, Dr. Robert Goldschmidt, Dean of Touro’s Lander College of Arts & Sciences, gave me a priceless piece of advice that I’ve used for decades. As an accounting major, Dean Goldschmidt knew I’d be in the business world and advised me to read the front page of the Wall Street Journal every day so I could stay on top of important news and developments and converse intelligently with colleagues. Dean Goldschmidt also said it would help me become a well-rounded person. That tip helped me as an accountant and I continued to follow his advice even as I moved into the health sciences. There are so many times that I need to break the ice with a patient or distract them from pain or a procedure and I do it successfully using something I read that morning as a conversation starter. It always works!
What advice would you give to the public about the pandemic?
Pay attention to health information and necessary precautions. Trust the health care professionals with current experience. We don’t have an ulterior motive, we all just want to minimize the spread, manage this horrific situation and keep people healthy. Maintain good hygiene, don’t break social distancing barriers, stay well hydrated and wear your mask. Don’t wait until someone close to you becomes critically ill or dies to take this seriously. Hopefully, these measures will help us all stay healthy!

